Does Cannabis Ease the Pain?
Today, WNBA star Britney Griner is flying home after serving 10 months in a Russian prison for possession of hash oil, a cannabis concentrate that had had been prescribed to her, legally, by an Arizona doctor for management of pain. In February, Ms. Griner had been arrested when Russian authorities found two vape cartridges containing a total of .702 grams (about .02 ounces) of the oil in her luggage. Welcome home, Britney.
One of the topics I'll be addressing in this newsletter is whether doctors should be prescribing cannabis products for pain relief. The question is whether cannabis reduces pain safely, and, if so, what mechanism underlies its effects? In order to get to this question, I need to talk first about the relationship between scientific studies and public awareness of the results.
A challenge
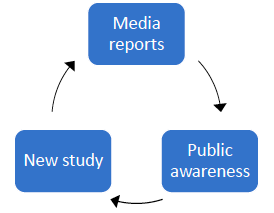
Whenever a new study is published, we assume that people might hear about the findings through sources such as news and social media:
In a flowchart like this, you wouldn't add an arrow leading from "Public awareness" back to "New study", because it's impossible for public awareness of a study's findings to somehow travel back in time and influence what the researchers find.
However, when a new study examines a topic addressed in prior research, participants in the new study may be "contaminated" by what they've heard about the earlier findings.
To illustrate how this works and why it's important, I'll be discussing a meta-analysis, published last week, that looks at whether cannabis is effective at reducing chronic pain. The findings suggest a placebo effect – people report that cannabis reduces pain simply because they expect it to do so. But where did they get that expectation? Apparently from media coverage of earlier studies on the same topic. The media reports indicate that cannabis reduces pain, but they don't necessarily mention placebo effects.
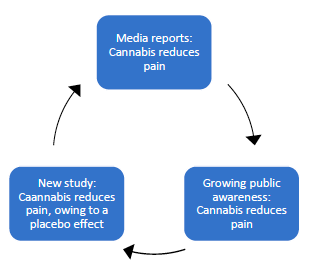
What I'm describing here is a kind of self-perpetuating cycle. People hear from the news that cannabis relieves pain. Later, those who participate in a newer study report that cannabis reduces their pain, because that's what they expect to happen. The newer study is then described in media reports that influence future study participants, and the process continues:
Cycles like this pose a challenge for researchers, because they increase similarities between new findings and older ones but obscure the underlying mechanisms. If everyone believes that cannabis reduces pain, and that belief has a placebo effect, then we may conclude that cannabis is an effective pain-reliever, but we don't know whether its effectiveness is just a placebo effect, or whether its chemical properties also play a role. At the end, I'll explain why this distinction is critical.
Quick terminological note
Here's are some terms that will crop up in this newsletter:
"Cannabis" is a genus of plant consisting of three species (C. sativa, C. indica, C. ruderalis).
"Marijuana" is a term for cannabis that's psychoactive (i.e., gets people "high"). This is generally C. sativa, C. indica, or a hybrid.
"Cannabinoids" are chemical compounds in cannabis. The two main types are "tetrahydrocannabinol" (THC), which is psychoactive, and "cannabidiol" (CBD), which is not.
"Hemp" is any cannabis product containing less than 0.3% THC and thus not psychoactive.
Practically speaking, we can treat "cannabis" as a broad category that consists of psychoactive substances (marijuana and THC) and non-psychoactive substances (hemp and CBD).
("Hash oil", such as what Britney Griner had been arrested for, is a cannabis concentrate that contains both THC and CBD.)
Background for new meta-analysis
"Leading medical researchers are coming to the conclusion that marijuana – pot, grass, whatever you want to call it – is probably the most dangerous drug in the United States." (Ronald Reagan, 1980.)
Researchers never did come to that conclusion. Rather, the effects of cannabis are turning out to be complex, and not all bad. For example, in the past nine months alone, studies have shown that cannabis use makes a person more prosocial (i.e., kinder) in the short-run, although people who use marijuana all their lives may show mild cognitive deficits in midlife and old age, and those who prefer to smoke it may have a greater risk of developing emphysema than those who smoke tobacco alone.
These studies add to existing evidence about the risks and benefits of cannabis use. Thanks to prior research, medical marijuana can be legally prescribed in 38 states now for problems such as nausea, anxiety, and pain. CBD products are available in most states as a dietary supplement based on claims, not well-substantiated yet, that they can alleviate stress, anxiety, inflammation, and pain. In addition, CBD is an FDA-approved treatment for certain rare kinds of epilepsy.
Much remains to be learned about the impact of cannabis on mental and physical health, because it's still classified as a Schedule I drug (along with heroin, meth, fentanyl, etc.), meaning, among other things, that researchers have to obtain a special license to administer it for the purpose of studying its effects.
This is a case where federal law lags behind the science. The Controlled Substances Act – passed in 1970 – defines Schedule I drugs as those "with no currently accepted medical use and a high potential for abuse". In fact, cannabis does have currently accepted, evidence-based medical uses. As to whether marijuana in particular has a high potential for abuse, that depends on how one defines "abuse", but studies do show that it's far less physically addictive than most Schedule I drugs, even though the neurobiological mechanisms of addiction may be similar. (CBD is not psychoactive, and thus not addictive in a physical sense.)
Although traditionally understudied, you'll be seeing a lot more cannabis research in the near future, thanks to two legislative changes:
First, in 2018, the Farm Act Bill removed hemp from Schedule I classification, which immediately enabled administration of CBD in experimental studies.
Second, on Friday of last week, President Biden signed into law the Medical Marijuana and Cannabidiol Research Expansion Act, a bill that increases researchers' access to marijuana (for scientific study). Marijuana remains a Schedule I substance for now, but the impact of this new law, along the Farm Act Bill, will be a higher volume of research into both marijuana and CBD.
This brings me to a new meta-analysis looking at the impact of cannabis on chronic pain. (A meta-analysis is a kind of review that uses statistical methods to synthesize prior studies on a topic.) Although cannabis products are currently prescribed for chronic pain – and widely believed to be effective – this new analysis questions whether it's actually cannabis that helps.
New meta-analysis: Methods
The new meta-analysis, conducted by a Swedish research team, was published in JAMA Network last week. A total of 20 studies (1,459 people) were analyzed. In each study, people seeking treatment for ongoing pain either received cannabis or a placebo. They also rated their pain on a simple numerical scale at the beginning and end of the study.
I mentioned that about half of the people in each study "received cannabis"? What does that mean exactly? Did a research assistant hand each person a joint and a lighter?
Well, yes, in one study, that's what happened. In the other 19 studies, cannabis was provided in the form of spray, vapor, pill, or oil. The studies ranged in duration from 45 minutes to over 12 weeks. The actual substance people received in some some studies was marijuana, or, more commonly, THC, while in other studies it was a synthetic cannabinoid (dronabinol or nabilone), or an extract (Nabiximols) – all of which are psychoactive. In three studies, the substance was CBD.
In short, the 20 studies varied widely in methodology. Is this a problem? The researchers ran analyses showing that differences in form of delivery, duration of study, and type of substance had no impact on the results. However, they didn't report the details of those analyses, and it's possible they were underpowered – in other words, with only 20 studies, the sample might not have been large enough for the necessary comparisons to be meaningful. It seems important to know whether psychoactive forms of cannabis outperform the non-psychoactive form (CBD), for instance, but CDB was only used in three studies.
Luckily. the findings were so consistent across the 20 studies that variability in their methods doesn't seem to matter. More on this in a moment.
New meta-analysis: Main findings
By the end of each of the 20 studies, participants tended to report less pain, regardless of whether they'd received cannabis or a placebo. The two groups did not differ significantly in extent of pain reduction.
This finding suggests that the reason cannabis reduces pain is, at least in part, because people expect it to. This finding is not unprecedented – other studies show that expectations for how much pain we're going to experience influence how much of it we actually do experience. (If you can somehow convince yourself that your dental procedure won't hurt much, it may not hurt much.)
A key assumption here is that even though study participants don't know which substance they'd receive, they did know that cannabis is a possibility. The fact that placebo effects emerged across studies varying so much in methodology increases our confidence that we're looking at a general phenomenon rather than one that occurs only for particular forms of delivery or particular types of cannabis.
So far I've shared with you a fairly standard, well-executed meta-analysis. It's a little light on details, but I have no major concerns. There is, in addition, a clever twist introduced at the end.
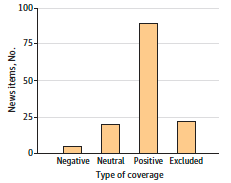
The researchers used a digital tracking service called Altmetrics to examine how the 20 studies were cited in media reports. They obtained 136 reports and rated each one in terms of whether the connection between cannabis and pain reduction was described in the report as positive, negative, or neutral. The researchers found that most reports were positive, regardless of how much pain reduction was experienced among the cannabis and placebo groups.
(In the figure above, "Excluded" refers to media reports that were not presented in English, or only appeared online as a temporary link.)
In short, news and social media help create the impression that cannabis reduces pain. In a sense, this is accurate, because it's what the studies show. But it's also misleading, because placebos seem to reduce pain to the same extent. This suggests that it's not the chemical properties of cannabis that help with pain but rather the media-created expectation that it will help.
In terms of the cycle I described at the outset, here's what seems to be happening:
One way researchers could break this cycle is to ask study participants about their expectations concerning the analgesic properties of cannabis. This could be as simple asking them to use a 7-point scale to rate the likely effectiveness of cannabis at reducing pain. Statistical analyses could later control for participant responses and give us a "purer" sense of how well cannabis works, apart from any expectations people have about it.
Conclusion
Should doctors continue to prescribe cannabis for chronic pain? And, in the 12 states where that's not a legal option, should people with chronic pain continue to take cannabis illegally if they feel it helps?
In my opinion, the answer to both questions is yes. It doesn't matter whether cannabis reduces pain through placebo effects, pharmacological mechanisms, or some combination of the two. If it works, it works, and I wouldn't want to deny this benefit to someone who experiences chronic pain. Take the drug, I'd say. Just don't take it to Russia.
Meanwhile, it's important for scientists to break the self-perpetuating cycle I described, so that placebo effects can be distinguished from any pharmacological benefits. If the pain relief is all a placebo effect, then there's no reason to continue studying specific compounds and forms of delivery. However, if there are genuine pharmacological effects, then researchers can focus on enhancing them. Perhaps not all compounds or forms of delivery are equally effective. Or, perhaps we're not even looking at the right compounds. In a 2019 study, Italian researchers discovered by accident two new cannabinoids called tetrahydrocannabiphorol (THCP) and cannabidiphorol (CBDP), and THCP in particular turns out to be much more potent than THC.
How is it that researchers are only now discovering new cannabinoids? Well, there are roughly 150 of these compounds (including terpene, closely related to the one that gives your Christmas tree its "piney" smell), but these chemicals are difficult to isolate. Apparently, new methods are making this process easier. These methods, combined with relaxed legal restrictions, make it likely that we'll know much more about the connection between cannabis and pain in the near future.
Thanks for reading!