Food Ambivalence
"Sooner or later, everything solid you thought you knew about the links between diet and health gets blown away in the gust of the latest study." (Michael Pollan, Unhappy Meals, 2007.)
How long have we felt ambivalent about what we eat?
I mean, how long have we chosen something from a menu or grocery store shelf or fridge and thought, oh, that has way too much (or too little) of something, but it's going to be tasty? How long have we eaten things that aren't tasty because we thought they're nutritious? In short, when did we start to be at odds with our food?
Here's a clue: In the past couple of months, we've seen new studies on the health impacts of the Mediterranean diet, the Atlantic diet, the Keto diet, olive oil, fish oil supplements, ultra-processed foods, high-fat diets, and intermittent fasting. In the past week, one study warned that low levels of vitamin B6 impair cognition, while another one questioned the safety of xylitol. A study published today links the Mediterranean diet to better reproductive health following a COVID-19 infection. Most of these studies made national news, and this is only a partial list. We are perpetually supersized with data on what to eat, and, as Michael Pollan notes, the new findings keep changing what we thought we knew. We have many opportunities for ambivalence.
Before we felt that way, we argued with each other, Nearly 2,000 years ago, Galen remarked that "One can find many people making the most contradictory statements about the same foods", an observation that seems to have applied to every historical period since then. So, when was ambivalence added to the mix?
The origins of food ambivalence
Galen, by far the most influential physician of his time, dispensed observation-based nutritional advice grounded in humoral theory (e.g., he noted that cucumbers may cause a cold, thick humor to accumulate in the veins and lead to congestion). In contrast, we have been "statisfied" in the way we think about food, and this is where much of our ambivalence begins.
Specifically, nutrition science emerged in the early 20th century and soon began to links diet to health via statistical procedures developed around the same time. For the first time in history, our food choices were informed by more than just cultural traditions or the theories and personal observations of physicians. We had data now, gathered in some cases from tens or hundreds of thousands of fellow eaters. But this buffet of information quickly became messy and unsatisfying.
Consider, for instance, the humble egg. I like mine the way my Chinese friends make them: Scrambled in oil with chopped scallion and a dash of salt. But when I think about eating eggs, a tiny, data-driven voice in the back of head launches a monologue that goes something like this: Have some eggs: They're loaded with protein and other nutrients. Skip the eggs: They're high in cholesterol. Have some eggs anyway: Dietary cholesterol barely influences blood cholesterol levels. Skip the eggs: You may be one of those few exceptions to the rule. Have one egg then: Some studies show no effects of eating one egg a day. No, have two eggs: a study reported this March showed that as many as 12 per week fails to raise cholesterol levels. But maybe just one is safer: The study was small (140 participants) and only lasted four months....
I don't actually hear voices in my head, but you get the idea. It would be nice to eat eggs – or not eat them – without letting whatever we happen to know about nutrition make the experience so complicated.
In this newsletter I want to share with you a new study on the Planetary Health Diet, a relatively innovative approach to eating intended to promote the health of the planet as well as its people. At first glance, the study seems methodologically limited and unlikely to reduce any ambivalence you might have about food. However, I believe that by leaning into its limitations, we can actually gain some insights on how to reduce ambivalence and maintain a simpler perspective on eating.
The Planetary Health Diet
In recent years, food ambivalence has come to include not only concerns about the healthiness of what we eat but also the environmental impacts of food production. (Skip the eggs: They cause greenhouse gas emissions and water pollution. Have an egg anyway: They're nowhere near as bad for the environment as beef...)
In 2019, the prestigious medical journal The Lancet published a report from a commission of 37 experts representing 16 countries and supported by the non-profit organization EAT. The EAT-Lancet report, as it came to be known, is a science-driven policy recommendation motivated by the assumption that "Food is the single strongest lever to optimize human health and environmental sustainability on Earth."
Why is food so important? Because, as the EAT-Lancet commission points out, "unhealthy diets now pose a greater risk to morbidity and mortality than unsafe sex, alcohol, drug and tobacco use combined. Global food production threatens climate stability and ecosystem resilience and constitutes the single largest driver of environmental degradation and transgression of planetary boundaries."
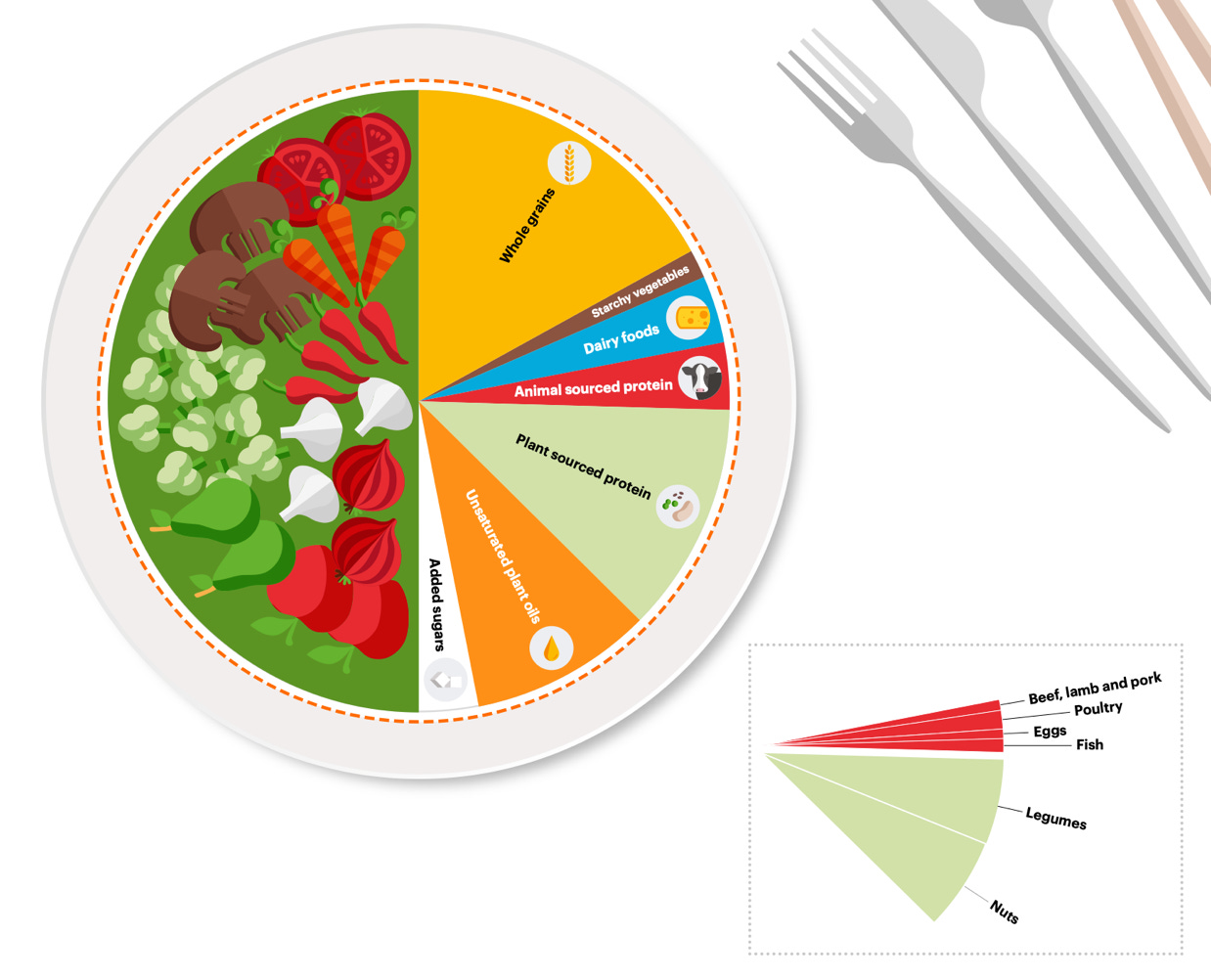
The commission concludes that we need a radical transformation of our food systems. To that end, they propose the Planetary Health Diet (PHD), which they define as follows:
"A planetary health plate should consist by volume of approximately half a plate of vegetables and fruits; the other half, displayed by contribution to calories, should consist of primarily whole grains, plant protein sources, unsaturated plant oils, and (optionally) modest amounts of animal sources of protein."
The commission presents this as a "flexitarian" diet, noting that "[l]ocal interpretation and adaptation of the universally-applicable planetary health diet is necessary and should reflect the culture, geography and demography of the population and individuals."
I would say this diet is even more flexible than the commission lets on. For instance, "half a plate of vegetables and fruits", by volume, could mean very different things. Half a plate of iceberg lettuce will be far less nutritious than the same amount of kale, not mention harder on the environment (owing mainly to heavier water requirements). Anyway, are everyone's plates the same size? What about bowls?
The Eat-Lancet report does offer some specific goals, such as 200 to 600 grams per day of vegetables, but it's hard to translate goals like that into practical advice given that (a) people differ in nutritional requirements, (b) we rarely weigh our foods, and (c) preparation methods matter. (Compare, for instance, equal amounts of kale chips versus fresh kale.) In sum, the Planetary Health Diet present a rough overview of eating patterns that would be most healthy for people and the planet. That alone makes it valuable, even if it doesn't list exactly what to have for breakfast.
The New Study
On June 10, the new study appeared on the American Journal of Clinical Nutrition website. The lead author, Linh Bui in the Department of Nutrition at Harvard, kindly shared the in-press version with me. (Senior author Walter Willet, also at Harvard, co-chairs the EAT-Lancet commission.)
The purpose of the new study was to develop the Planetary Health Diet Index (PHDI), a measure of how closely a person's diet resembles the Planetary Health Diet, and then check whether PHDI scores would predict mortality rates among older people. In short, would higher PHDI scores be associated with a longer lifespan?
Right off the bat, this looks like a potentially useful study for anyone who prefers their nutrition advice to be nuanced. By calculating PHDI scores, people can be said to be complying to a greater or less extent with the Planetary Health Diet. This seems more sensible than a simplistic contrast between being "on" versus "not on" the diet, especially given that the diet itself is flexibly defined.
(Of course, if you want concrete recommendations, they're easily found too - e.g., a short piece in the New York Times this Tuesday gets into the weeds – or greens, I should say – of a "perfect desk lunch" and even provides recipes.)
Methods and findings
Bui and colleagues analyzed data from three of the largest studies ever conducted on how nutrition impacts health in later life. Specifically, the researchers sampled 66,692 female nurses from the Nurses' Health Study I, 99,438 female nurses from the Nurses Health Study II, and 47,274 male health care professionals from the Health Professionals Follow-up Study. Data were gathered for the time periods 1986-2019, 1991-2019, and 1986-2019, respectively, and PDHI scores were based on how much of each of 15 food groups people report eating. (I've listed these food groups in an Appendix at the end.)
The main finding was that higher PHDI scores were associated with a lower risk of death. Statistically, the effects were small, but people in the top quintile (i.e., top 20%) of PHDI scores were 23% less likely than those in the lowest quintile to die during the study period, a pattern that was also seen for specific causes of mortality such as cardiovascular disease and cancer. Importantly, the link between PHDI scores and mortality emerged after controlling for key health variables such as hypertension and cholesterol levels, as well as key lifestyle variables such as smoking, drinking, and physical activity. The diets of people in the top PHDI quintile also implied significantly lower greenhouse gas emissions, as well as less water, fertilizer, and cropland use during the production of their food.
In short, Bui and colleagues' data suggests that hewing more closely to the Planetary Health Diet guidelines fosters better public and planetary health.
This is compelling, historically unprecedented data. Only in the past few decades have we had the statistical frameworks, the internet connectivity, and the sheer computing power to survey the eating behavior of more than 200,000 people and track their mortality rates over a roughly three-decade period.
Alas, this is the last unqualifiedly positive thing that can be said about the study. A closer look reveals both methodological and moral concerns.
A methodological issue
As with other longitudinal studies linking diet to health, we don't know clearly what participants ate, because they were only surveyed once every four years.
Once every four years. No survey administered that infrequently could yield accurate data. It's hard enough to get a precise read on what people ate last week – not just because they forget or fudge, but because nobody weighs their food or keeps track of every ingredient. Meanwhile, not that many people eat the same thing day after day, year after year, for any one meal, much less all of them.
You might argue (as the authors imply at one point) that lack of precision only makes the results more believable. Detecting a signal in spite of so much noise implies a strong signal. Here's an analogy: If you glance through a smudged window and guess that the building is on fire, your guess acquires a bit more credibility by virtue of the fact that you noticed signs of fire in spite of the smudging and the briefness of your glance.
This argument doesn't hold up well, either statistically or in light of the way science is routinely practiced. The statistician Andrew Gelman has borrowed the title of a Borges story, "The Garden of Forking Paths", to refer to the many different ways researchers can choose to organize and analyze the same dataset. Some paths may lead to significant findings, others may not. In his blog, Gelman is fond of providing examples of forking path practices that lead to questionable conclusions.
In this case, the researchers focused on PHDI quintiles, barely exploring what might've happened if they treated PHDI scores differently (e.g., as raw scores). They didn't justify their quintile approach, much less explain why they based PHDI scores on 15 food groups and not others (see my Appendix for the list). Why sugars but not sodium? Why combine red meats and processed meats into one category? Why exclude other processed foods? In the end, the researchers made dozens of decisions about data analysis that weren't explained, and we have no way of knowing whether paths other than those they took would still lead to associations between PHDI scores and mortality rates.
All this by way of saying that when a small effect is found in messy, imprecisely measured data, the fact that the measurement is imprecise doesn't necessarily justify more confidence in that effect. For all we know, the effect might disappear if the data had been analyzed differently. What you thought was a fire viewed through the smudgy glass might just be a ray of light reflected off a mirror.
(More on methodology at the end of the Appendix.)
A moral issue
Not everyone has the luxury of ambivalence. Approximately 14 million Americans experience food uncertainty (i.e., limitations on access to adequate food), and globally, nearly a billion people contend with this problem.
The 2019 EAT-Lancet report acknowledges the issue, arguing that the solution is to intensify food production (and to do so sustainably, under the assumption that a healthier environment translates into better standards of living for poorer people).
However, there is an alternative perspective. A 2020 Global Food Security article, for instance, suggests that animal source foods (meat and dairy) are the best way to meet the immediate nutritional needs of many of the world's undernourished people, because these foods are nutrient-rich, and, in some places, they're the most accessible options.
One of the concerns these authors raise about the Planetary Health Diet is that by recommending less consumption of animal source foods, the EAT-Lancet commission may be jeopardizing the health of undernourished people. If you're an American eating steak six nights a week, you should cut back, but if you're an undernourished mother in a developing country, the most effective (and perhaps accessible) solution to the problem is more meat and dairy for you and your infant.
Can you trust the authors of this 2020 study? The "competing interest" section of the article consists a single sentence: "Authors acknowledge no conflict of interest to report." In fact, every one of the five authors is affiliated with the Feed the Future Innovation Lab for Livestock Systems at the University of Florida. (I suppose it's true then that there's no conflict of interest: They're all pro-animal food. But that doesn't necessarily undermine what they have to say.)
In my view, what the University of Florida team adds to the EAT-Lancet report is the qualification that you can't save the world with a one-size-fits-all approach. For humanitarian reasons, beef production may need to increase in some parts of the world, at least temporarily, while being scaled back elsewhere.
Bottom line
Given the methodological limitations I described above and in the Appendix, I don't see the data as either supporting or disconfirming the new study's conclusions. Perhaps the best that can be said for the Planetary Health Diet, at the moment, is that it was designed by the Eat-Lancet commission on the basis of reputable data, and it resembles the Mediterranean diet, which has been shown to be relatively healthy for the planet and its inhabitants. (Side note for stats people: The researchers used the Mediterranean diet and others as covariates, but failed to take the obvious step of checking to see how well each diet worked as a predictor. Clearly a missed turn in the garden of forking paths.)
How to overcome food ambivalence
The message of the new study, if you could trust the data, would be that the more your food choices resemble the Planetary Health Diet, the longer you'll live. But guidance on what to eat remains a bit vague, and the findings don't seem positioned to reduce food ambivalence, because they still discourage consumption of foods many of us love (e.g., meat and dairy), while recommending more vegetables and other foods some of us view less enthusiastically.
Marketing studies have shown that people assume healthier foods are less tasty, while tastier foods are less healthy, so food ambivalence may reflect a general bias rather than being tied to specific foods. Either way, I think we can address the ambivalence problem by leaning into the vagueness of Bui and colleagues' findings. Instead of trying to squeeze the data for concrete guidance about what to eat, we can simply acknowledge that this study (and others like it) merely hint at what a healthy diet would look like.
My takeaway then is that we should relax. Eat more veggies. Eat fruits and nuts. Cut back on meat and dairy. Cut back on processed foods and additives such as sodium and refined sugar. But don't set targets unless you're comfortable doing so, and don't stress about day to day consumption. Don't get caught up in Tik Tok fads or U.S. News rankings either (yes, U.S. News ranks diets too).
This is analogous to what I've suggested about the 10,000 step rule: We should try to stay active, but not count steps, because the data doesn't point to anything especially beneficial about the 10,000-step-per-day mark, or any other particular step count. Statistical procedures evolved as a way of measuring and managing uncertainty, but statistics don't necessarily resolve uncertainty. We should move around more and eat healthier, but not fret over specifics that the data is inherently unable to address.
The 2019 Eat-Lancet report describes itself as "the first attempt to set universal scientific targets for the food system that apply to all people and the planet." That's laudable, but it doesn't offer much guidance on what you should be eating for breakfast tomorrow. Steak may be perfectly fine. So might Rice Krispies with extra sugar. Perhaps these would be healthy options every day of your life, if portion sizes were small and the rest of your meals were healthy and environmentally sustainable. The key point is to enjoy your food, and to try to eat well without stressing over whatever efforts you're making to do so.
Thanks for reading!
Appendix: The 15 food groups used in Bui et al. (2024), and one more methodological issue
–Whole grains
–Tubers
–Vegetables
–Whole fruits
–Dairy foods
–Red/processed meats
–Poultry
–Eggs
–Fish/shellfish
–Nuts
–Non-soy legumes
–Soy foods
–Added unsaturated fats
–Added saturated fats and trans-fat
–Added sugars and sugar from fruit juices
The 2019 EAT-Lancet report has been criticized (in The Lancet, for instance) for omitting key information of vital importance to interpreting the findings. The same criticism applies to the new study.
In particular, each of the 15 food groups listed above was assigned a score of 0 through 10 (or in a few cases, 0 through 5). Higher scores correspond to more healthy eating – e.g., eating no vegetables at all, or way too much red/processed meats, would be coded as a 0 for each of those food categories. Scores were then totaled and, as I mentioned, statistical analyses focused on quintiles.
Here's a startling detail: Nowhere in the article or the supplemental materials do the researchers explain how those scores were assigned. They merely allude to "dose-response relationships", meaning that for each particular food, they first looked at data on the relationship between amount consumed and health impacts, and then decided how much of the food would justify a score of 1, versus a score of 2, a score of 3, and so on all the way up to 5 or 10. We have no idea what paths were chosen in the assignment of scores,
This is a key omission. It's hard to glean practical guidance from this study without knowing how the scores were derived. Sure, higher scores for vegetables are desirable, but what score should you aim for, and what does each score mean? How much more veggies do we have to eat to increase our chances of living longer? How much less red/processed meat reduces our risk of mortality? In the end, the study gives us nothing but the recommendation to eat more of the good stuff and less of the bad. Sound advice, but we knew that already.